Kneecap Instability or Dislocated Knee:
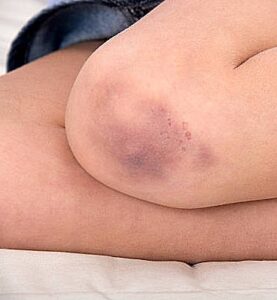 Patellar instability, also known as kneecap instability, occurs when the patella (kneecap) falls out of the thighbone’s femoral groove. Therefore, an unstable kneecap can cause a dislocated knee. Physical therapy and leg braces may help. Unfortunately, kneecap instability is a condition that affects certain people on a long-term basis. The trochlear groove is a V-shaped notch on the kneecap that glides up and down when you bend and straighten your knee. Kneecap instability causes the kneecap to not track properly in the groove. Consequently, dislocated knees, ACL rupture, and arthritis in the knee are all risks associated with this illness.
Patellar instability, also known as kneecap instability, occurs when the patella (kneecap) falls out of the thighbone’s femoral groove. Therefore, an unstable kneecap can cause a dislocated knee. Physical therapy and leg braces may help. Unfortunately, kneecap instability is a condition that affects certain people on a long-term basis. The trochlear groove is a V-shaped notch on the kneecap that glides up and down when you bend and straighten your knee. Kneecap instability causes the kneecap to not track properly in the groove. Consequently, dislocated knees, ACL rupture, and arthritis in the knee are all risks associated with this illness.
What’s the Connection between a Dislocated Kneecap and Kneecap Instability?
A displaced kneecap can result from kneecap instability, and the result may be:
- Complete dislocation: The ligaments holding the kneecap in place slip to the outside of the knee, dragging the kneecap after them. Ligaments can get torn or stretched. The kneecap appears out of position.
- A partial dislocation (subluxation): The kneecap comes out of the groove slightly.
- A dislocation of the kneecap is referred to as a dislocation. The thighbone (femur) and the shinbone (tibia) are involved in a “dislocated knee” (tibia). The femur and tibia do not connect at the knee joint when the knee is dislocated. One of the bones has been pushed backward or forward in comparison to the other. Because of the force necessary to misalign the leg bones and the damage it causes to the ligaments, a dislocated knee (tibiofemoral dislocation) is uncommon and more dangerous than a dislocated kneecap.
Patella Dislocation Affects Who?
- Athletes, particularly those who participate in high-impact sports, are more vulnerable.
- Dancers who are prone to pivoting quickly.
- Teenagers, whose ligaments and joints are looser as a result of continual growth.
- Women with larger hips and loose ligaments.
- Big and tall guys who have extra pressure on their joints.
- People with patellar instability, particularly if their patella has already dislocated.
Doctors aren’t sure what causes congenital patella dislocation, but the fact that it occurs more frequently in family members implies a hereditary relationship. It’s also linked to several other congenital diseases, including:
- Larson Syndrome.
- Diastrophic Dysplasia.
- Nail-Patella Syndrome.
- Down syndrome
- Ellis-Van Creveld Syndrome.
How Common Is Kneecap Instability?
Throughout the day, children are frequently on their knees. As a result, they are more susceptible to issues such as patellar instability. According to experts, 50 to 77 Americans out of 100,000 have some form of patellar instability.
What Causes Instability in the Kneecap?
The skeletal system includes the kneecap. The front of the thighbone (femur) has connective tissues that travel over the kneecap and attach to the shinbone (tibia). When your child straightens his or her leg, these muscles pull the kneecap up through the trochlear groove, and when your child bends it, they draw the kneecap down through the groove. The kneecap slides outside of this groove when it is unstable.
A Variety of Factors can Cause Patellar Instability, including:
- A shallow or irregular Trochlear groove.
- Joints that are overly flexible or ligaments that are excessively loose.
- A fall, sports injury, or another event can result in a severe impact on the kneecap.
What are the Things that Put a Kneecap in Jeopardy?
Patellar instability can affect anybody. Females’ ligaments are looser, making them more prone to patellar instability. If your child participates in high-impact sports like football or activities that demand a lot of fast rotation, such as basketball, cheerleading, or soccer, your child may be at a higher risk. In addition, loose connective tissue caused by certain health issues can cause Patellar instability. These are some of them:
- Cerebral palsy
- Down syndrome.
Does a Displaced Kneecap Cause Pain?
Dislocations are frequently very painful; however, there is a wide spectrum of suffering. It depends on how far out of the joint the bone has been pressed, as well as the extent of injury to the surrounding muscles and ligaments, blood vessels, and nerves. It will always hurt to move or bear weight on a displaced joint. Until the joint is repaired, your child won’t utilize the limb normally. Your child’s pain, discomfort, and mobility may improve if the displaced patella heals on its own. However, you should still take your child to visit a pediatric orthopedist to ensure everything is ok. They’ll look for subsequent ligament problems and walk the parents through the lengthy recovery process.
How do you know if your Child has Kneecap Instability?
Even if your child’s kneecap returns to its original position on its own, parents should consult with their doctor for diagnosis and treatment options. Your doctor will conduct a physical exam to examine the knee and listen to the patient’s symptoms.
Your child may also get:
- X-rays to check for shattered bones and examine whether the kneecap is out of place.
- An MRI is used to look for injuries such as ACL tears, meniscal tears, and loose bone fragments.
By physically inspecting the knee and asking the parents questions regarding the incident, knowledgeable healthcare experts can typically identify a dislocated kneecap. They will, however, conduct radiographic imaging tests to rule out any linked ailments such as torn ligaments, cartilage damage, or fractures. When it comes to patellar dislocation, it’s best to treat the joint first and then take photos. Parents might not recognize that their child’s displaced patella was dislocated if it fixed itself. “Transient” refers to a dislocation that corrects itself. Your child’s knee will remain uncomfortable and swollen thereafter, although it may resemble a variety of other, more typical knee problems. In this situation, imaging studies might reveal indications of dislocation as well as subsequent damage after the event.
Non-Surgical Options for Treating Kneecap Instability or a Dislocated Knee?
Seek medical help if the kneecap does not return to the trochlear groove on its own. The doctor will gently push the kneecap back into position. This procedure can be unpleasant, so your child will be given mild pain medication, but anesthesia is not required.
If your child has a partial knee dislocation or patellar instability, your doctor may suggest:
- A knee brace helps hold the kneecap in place while immobilizing the knee. Your child may need to use crutches and wear a brace for many weeks.
- To relieve pain and swelling, Nonsteroidal anti-inflammatory medications (NSAIDs), rest, elevation, and cold packs are used.
- Physical treatment helps enhance the range of motion and strengthen the muscles that keep the kneecap in place.
Surgical Options for Treating Patellar Instability
Depending on the etiology of the instabilities, there are several therapy approaches. Knee arthroscopy can assist with cartilage injury by removing loose pieces or reattaching the cartilage when possible. Surgeons may also release tissues that are interfering with the kneecap’s natural mobility or push the kneecap off track during the treatment, allowing the patella to track normally once again. Your healthcare professional may prescribe surgery if your child has persistent patellar instability or complete kneecap dislocation. The majority of knee procedures are performed arthroscopically. Small incisions and a tiny camera are used in the surgery (arthroscopy). Recovery might take anywhere from six to twelve months. If your child has patellar instability as a result of an accident, your child may have loose cartilage or bone fragments in his or her knee. The surgeon may surgically remove bone fragments.
Surgical options include:
- The ligaments that keep the kneecap in place are strengthened and repaired during medial patellofemoral ligament (MPFL) surgery.
- A hamstring tendon from a donor or from somewhere else in your child’s body is used to repair a damaged ligament in the MPFL.
- Realign the shinbone, thighbone, kneecap, and connective tissues using a knee osteotomy (tibial tubercle transfer). In comparison to arthroscopic surgery, open surgery necessitates a wider incision and a longer recovery time.
- Knee replacement is used to treat severe arthritis or recurring dislocations in the knee.
What can I do to Avoid Kneecap instability?
Connective tissue can get damaged by an unstable kneecap. Repeated kneecap dislocations are more likely to occur as a result of this injury. Muscles and connective tissue that maintain the kneecap in the femoral groove can be strengthened using physical therapy exercises. Cycling, whether on an exercise bike or outside on a real bike, is a fantastic way to improve your child’s knees. Your doctor may recommend wearing a knee brace during specific activities.
What is the Prognosis for Patients Suffering from Kneecap Instability?
Nearly half of those who undergo nonsurgical therapy for patellar instability will re-dislocate their knee. This indicates that the kneecap is still shaky. Your child is more likely to develop arthritis and ligament damage if he or she has chronic patellar instability. In this case, your doctor could suggest surgery.
When Should I Schedule an Appointment with a Physician?
If your child exhibits any of the following symptoms, you should see a doctor:
- The knee will not bend or straighten.
- It is difficult to put weight on the legs or walk.
- Knee pain or restricted range of motion that makes daily life difficult.
- The knee joint appears unusually red or swollen.
- The kneecap shifted and will not return to its proper position.
- Your child finds it difficult to elevate a leg independently.
- The injury gets worse with time.
- When your child’s knee catches and locks, and experiences pain.
What Questions Should I Ask My Doctor?
- What caused patellar instability in the first place?
- Is my knee partially or completely dislocated?
- What treatments can help?
- Is it possible to benefit from physical therapy or other exercises?
- Would surgery help?
- How can I avoid knee troubles or dislocations in the future?
- Should I look for signals of trouble?
A Special Note:
Patellar instability raises the likelihood of a knee dislocation. Ligament tears and arthritis are also possible outcomes. Wearing a brace and practicing physical therapy will help most individuals feel better without surgery.
We encourage questions and invite those who have read the information above to give us a call. The Medical City Children’s Orthopedics and Spine specialists dedicate our practice to helping children. We have offices in Dallas, Arlington, Frisco, and McKinney, Texas. We specialize in children and do not see adult patients. If you need an expert for your child’s illness or condition, we will provide the best-in-class care for your child. Pick up the phone and call us today.
____________________

Recent Comments